TMJ Treatment – Houston, TX
Restoring Comfortable Motion
for Effortless Smiles
"TMJ" is a popular buzzword in our society, which, in reality, is an acronym for an anatomical body part, the temporomandibular joint. "TMJ" is not a syndrome, nor a disease, but is merely a designation for the human jaw joint. To say someone "has TMJ" is the same as saying someone "has a knee." However, TMJ disorders are a major cause of facial pain and dysfunction and are an important and appropriate focus of attention by health care providers. TMJ disorders consist of a family of problems that relate to your jaw joint complex. These problems involve complicated anatomical structures such as muscles, ligaments, tendons, the mandible (lower jaw), teeth, nerves, blood vessels, and other structures. When your TMJ and associated structures are in good health, the jaws open and close smoothly and comfortably when talking, chewing, and performing other functions. We can restore this function with TMJ treatment in Houston, TX.
TMJ Anatomy
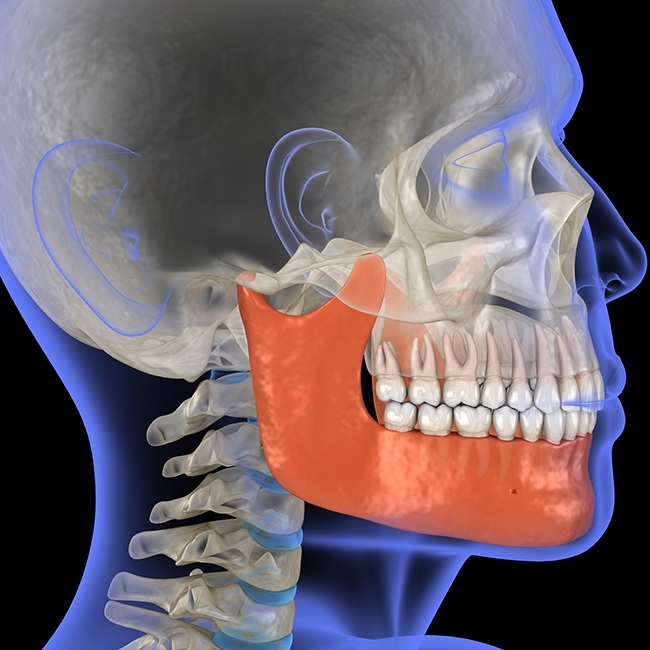
Complex Masticatory Muscles - Surrounding the joint are groups of muscles that contract and relax in harmony, so the jaws function properly. When the muscles are relaxed and flexible and not under stress, they work in harmony with the other parts of the TMJ complex.
Teeth and Occlusion - The way the teeth fit together may affect the TMJ complex. A poor occlusion (bite relationship) may cause the muscles to malfunction and ultimately cause damage to the joint itself. A stable occlusion with good tooth contact and interdigitation provides maximum support to the muscles and joints. Instability of the occlusion can increase the load or pressure on the joint causing damage and degeneration.
Temporomandibular Joint - The temporomandibular joint is the joint where the lower jaw articulates with the base of the skull and allows movement of the lower jaw. This joint is made up of the mandibular condyle which is the round end of the mandible that moves and rotates while talking, eating, etc. The temporal fossa is the socket where the condyle fits. The disc or meniscus is situated between the condyle and fossa and is made up of cartilage-like dense collagen. It provides the sliding action between the lower jaw and the fossa (or top part of the joint). Ligaments hold the disc to the condyle and help stabilize the joint. Connective tissue holds the disc to the back of the joint and contains blood vessels and nerves. Connective tissue also forms the joint capsule which surrounds the joint. The illustration above demonstrates the "normal" relationship of the disc to the surrounding joint structures. While many patients have discs that are displaced from this position and NOT have any symptoms, it is very common that those who have TMJ pain and dysfunction also have displaced discs. It is therefore likely that this displacement plays a significant role in the development of such problems.
Causes of TMJ Disorders

Trauma or Jaw Injury - This can cause injury to the joint in the form of fracture to the condyle, torn ligaments, torn cartilage, displacement of articular discs, damage to muscles and other injuries.
Diseases - Certain diseases such as rheumatoid arthritis can affect the joint surfaces and certain muscular diseases can affect function.
Stress - This is often the cause of TMJ pain. Stress can be manifested by clenching and overstressing the muscles and jaw joints. This can be seen as pain, muscle spasm, or damage to the joints.
Habits - Bruxism (grinding the teeth, especially at night) can cause muscle and joint problems.
Bite or Occlusion Problems - Misaligned teeth, missing teeth, and misalignment of the jaws can create an imbalance of muscular and joint function which can lead to discomfort and joint damage.
What to Expect During a TMJ Evaluation
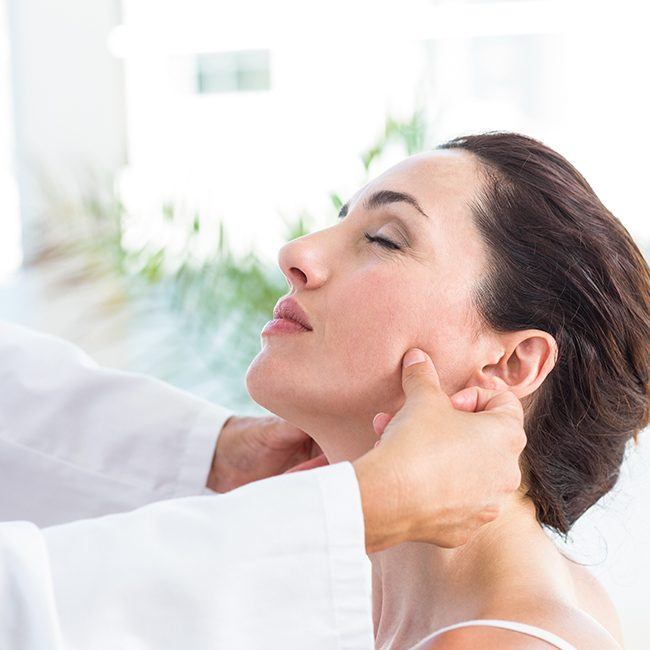
The first step to arriving at a TMJ treatment plan involves a fact-finding program. This collects the necessary information to arrive at a diagnosis.
Dental and Medical History - This provides information about your overall health, any history of accidental injuries, symptoms you are experiencing, treatment you have received, medication you are taking, and much more. It helps determine lifestyle, habits, stress factors, and family history. All of this information is important.
Physical Exam - This helps identify your symptoms and malfunctions. It may involve the examination of your muscles and joint for tenderness. Jaw function is carefully measured. The joint can be examined for noises and sounds by various listening devices. Your teeth and occlusion may be examined to determine the stability of your bite.
Imaging Tests - A variety of tests help confirm or rule out a diagnosis of temporomandibular joint disorders. Various x-rays (tomograms, transcranial scans, and others) show an image of bony contours of the joint. These films may reveal fractures, tumors, or damage to the bony surfaces of the joint. An MRI (magnetic resonance imaging) produces images of both hard and soft tissues and may reveal damage or displacement of the disc or ligaments.
Dental Casts - These are models of your teeth that may help determine if there is instability of your bite in relation to your disorder. It may also reveal a joint disorder that has affected the way your teeth fit and line up.
TMJ Diagnosis
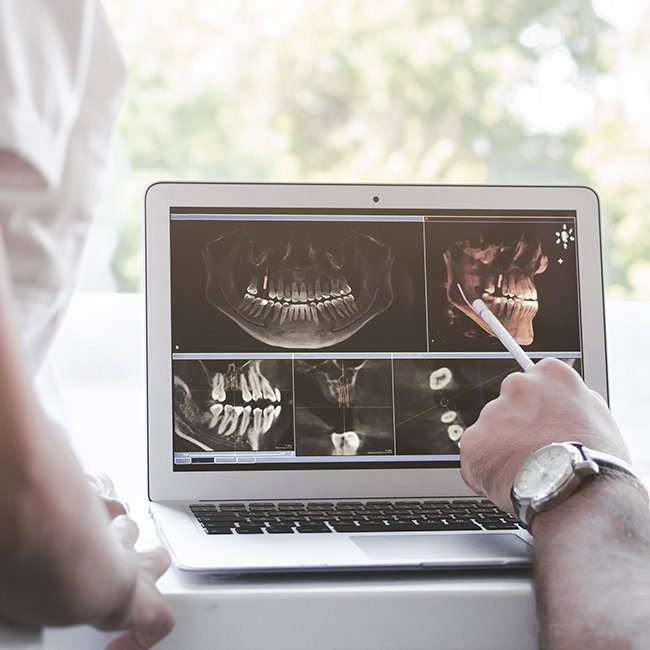
A good diagnosis is of primary importance, so the proper treatment may be precisely directed to the correct TMJ dysfunction.
Extracapsular Disorders - These are disorders that exist outside the joint itself. These patients often have little or no mechanical problems within the TMJ but suffer the effects of the structures outside of the joint.
Myofascial Pain Dysfunction - This is the most common TMJ dysfunction and usually involves muscle imbalance with muscle spasm and pain. This has a multitude of causes such as stress, grinding of teeth, instability of the bite, and others.
Diseases and Pathology of the surrounding area - This can include tumors of the jaw, salivary glands, and associated structures, neurological disorders, systemic disorders affecting the head and neck, and referred pain from the neck, back, and associated structures.
Internal Joint Disorders - Damage or disease to the joint itself such as the disc, condyle, ligaments, or synovium (lining of the joint).
Disc Displacement - A displaced disc may cause popping and clicking due to the disc being displaced forward so that the condyle clicks or pops in its translation when opening the mouth. A displaced disc may block the condyle from translating forward and restrict the opening. This is sometimes called a "closed lock."
Adhesions - Scar tissue may have developed between the condyle and disc or the disc and the fossa that restricts jaw movements.
Disc Perforations (holes or tears in the disc) - This occurs when the disc is torn or worn through by continually overloading of the joint. This often causes a grinding sensation or gravel-like sound.
Arthritic Conditions - Advanced wear and breakdown of joint surfaces causing pain, grinding noises, and general joint dysfunction.
Hypermobility - Sometimes the joint becomes too loose and the posterior ligament is structured to allow the condyle and disc to advance forward beyond the socket. This can cause the jaw to lock open. This is sometimes called an "open lock".
Synovitis - The synovial lining, which produces lubrication to the joint, may become inflamed for a variety of reasons. This often causes an acutely tender and painful joint.
TMJ Non-Surgical Treatment Options

Joint problems don’t always have to have surgical solutions. In fact, there are plenty of ways to relieve TMJ pain without invasive treatment. There are actually multiple treatment options to consider; before we make a recommendation, we’ll carefully examine your mouth, face, and jaw. Many of the below treatment options can be used in conjunction with each other in order to speed up your recovery and stop the discomfort as soon as possible. Be sure to let us know if you have questions about your treatment.
Self Help

This is usually the best option to begin with. Resting the jaw may be the best treatment, so the jaw joint can heal and regain stability. This may be accomplished by not clenching your teeth, practicing good posture, eating soft foods, and reducing stress. Apply ice to the jaw for the first 24-48 hours after symptoms are noticed. Ice helps prevent swelling. Heat may be applied to tense and sore muscles. By application of heat, muscle spasms may be relieved. Exercise (passive) of the jaw regains normal range and function. It increases flexibility and strengthens muscles. This should be done as a passive exercise in contrast to eating hard foods which increases the stress on the joint. Medications such as Motrin, Advil, aspirin, or other non-steroidal anti-inflammatory drugs reduce pain and inflammation.
Medications

Your doctor may prescribe muscle relaxants to decrease and control muscle spasms and muscle related pain. Non-steroidal anti-inflammatory drugs may be prescribed to reduce inflammation and control discomfort. Drugs to help control bruxism or grinding of the teeth may be recommended.
Physical Therapy
You may be referred to a licensed physical therapist to help in the management of your disorder. Physical therapy promotes healing and reduces pain, swelling, and inflammation. It greatly improves range of motion and muscle relaxation in the jaw. Physical therapy techniques may include jaw exercises, posture training, mobilization of joints, ultrasound, and electrical stimulation to regain harmony to your jaw joints and muscles.
Splint Therapy

It may be recommended that you wear a splint which is a clear plastic appliance. It fits over your teeth to help establish harmony between your muscles and joints. Splints primarily aid in stabilization of the bite and preventing and controlling bruxism and bite clenching. Most splints are constructed by your general dentist or a dentist who specializes in non-surgical TMJ management. Most splint therapy lasts for 1-3 months or more. A bruxism splint is worn primarily at night to prevent grinding and clenching habits. It helps to reduce muscle tension and discomfort. An orthopedic stabilization splint lets your jaw move into the correct position, stabilizes the bite, relaxes musculature, and reduces pressure on the TMJ. Proper wearing of your splint as directed by your doctor is most important in the treatment of your dysfunction. In the illustration at right, the splint is in place between the upper and lower teeth. It will act to perfect the bite artificially and prevent excessive force from being transmitted to the TMJ as the patient clenches or grinds. It will help with force dissipation even in the absence of these parafunctional activities and encourages the joints to repair themselves. The greatest advantages of this therapy are that most people will be helped to some degree, and the therapy is safe and reversible.
Occlusal bite correction
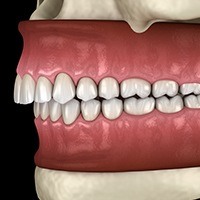
If your TMJ disorder is caused or greatly affected by the way your teeth fit together, it may be necessary to correct your occlusion. You may need orthodontics (braces) to reposition your teeth in order to establish a stable bite. If your bite problem is primarily due to a malalignment of the jaws or a discrepancy between the upper and lower jaws, you might need orthognathic surgery. This would realign the upper and lower jaws (usually in combination with orthodontics) to create a stable occlusion. Restorative dental procedures may be necessary from your general dentist to replace missing teeth, repair existing teeth, or change the shape and size of teeth.
TMJ Surgery
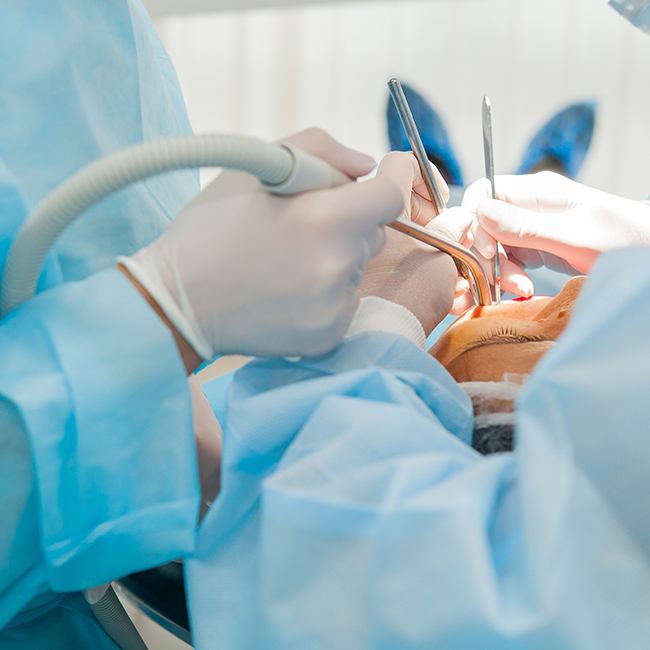
With other modalities of treatment available, surgery is reserved for those cases which fail to satisfactorily respond to the above-mentioned methods. In some cases, the joint undergoes some degree of internal joint derangement and fails to respond to non-surgical treatment. Surgery is usually indicated if non-surgical treatments have failed and clinical and diagnostic findings indicate a derangement inside the TMJ. The following are several different types of TMJ surgery:
Lysis & Lavage
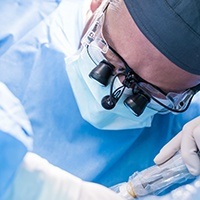
This is hydraulic distension and flushing of the joint with sterile saline and/or medications to increase the mobilization of the joint. If the disc has become adhered to the fossa surface or locked for a short period of time, this procedure may remobilize the disc. Lysis and lavage is an oral surgery office procedure performed under IV sedation, which may be used to decrease discomfort and inflammation.
Arthroscopic Arthroplasty & Surgery
This procedure is similar to arthroscopic surgery performed by orthopedic surgeons on the knee and other joints. This procedure is usually done in a hospital setting, requires general anesthesia, and is routinely done on an outpatient basis. Most TMJ derangements can be initially treated by arthroscopic surgery. Arthroscopic arthroplasty can be done as a diagnostic tool if the diagnosis is uncertain and non-surgical treatments have failed. Adhesions and scarring may be removed to increase joint mobility. If the disc is displaced causing painful popping or locking, a repositioning procedure can be accomplished arthroscopically. Until the last several years, this required an open joint procedure, but with the current state of the arthroscopic "arts," many discal repositioning procedures, including suturing of the disc itself, are performed without open surgery. In cases of more severe degeneration such as torn discs, discs with holes worn in them, or arthritic and degenerative joints, arthroscopic surgery is highly effective. This procedure requires a small 3mm incision over the joint in front of the ear. Through this incision, the arthroscope is inserted into the joint space. Additional needles may be placed to perform the necessary procedures.
Open Joint Reconstructive Surgery
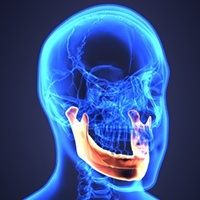
If the joint fails to respond to the arthroscopic procedure or the condition is such that arthroscopy is not indicated, an open procedure is sometimes recommended. Under direct visualization, the joint is reconstructed by smoothing the joint surfaces, repair of disc abnormality and removal of diseased tissue. A graft or artificial replacement of one or more joint surfaces may be used in the reconstruction of the joint. This procedure requires general anesthesia as well as an overnight stay in the hospital.
Condylotomy
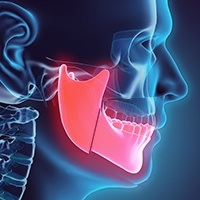
Sometimes the jaw is sectioned from inside the mouth and just below the condyle. This is done in certain situations to restore a stable occlusion, to decrease the pressure on the joint or to change the condyle position. This procedure requires having the jaws wired together for 7-14 days. It requires general anesthesia and an overnight stay in the hospital.
Follow Up Care After Surgery
Post-operative instructions will be given to you by your doctor regarding care of your incisions, suture removal, diet, physical therapy, and medications. Medication will be given for pain control, muscle relaxation, and prevention of infection. Additionally, postoperative physical therapy is an integral part of the rehabilitation after treatment. One of our doctors is always on-call for problems or questions and a postoperative appointment is usually scheduled 1-15 days after the procedure.
TMJ Treatment FAQs

If you are suffering from jaw pain and related symptoms, our team is ready to evaluate the situation and get you on the path toward relief. Before you book a consultation with us, though, you might be eager to learn more about TMJ treatment and what to expect from it. Below, you will find answers to some frequently asked questions about this service. If your specific questions are not included here, reach out to us directly — we look forward to speaking with you!
Can TMJ Be Cured Permanently?
Some forms of TMJ treatment are designed to provide fast but temporary pain relief. For example, lifestyle modifications and other home remedies can reduce discomfort. However, since they do not address the root causes of TMD, their effectiveness has a limited duration.
Other treatments address the underlying causes of TMD, so they have the potential to provide long-lasting results. If you do not suffer any additional injury or damage to your TMJ after you complete your treatment, you may enjoy permanent freedom from your symptoms.
How Long Does TMJ Treatment Take?
The timeline for TMJ treatment can vary. For example, an occlusal splint might provide results in as little as a few weeks, but some patients do not experience benefits for several months. If you undergo equilibration, you might experience results within just a few days. If you undergo corrective jaw surgery, you should begin to notice pain relief shortly after you recover from your procedure.
Can TMJ Be Treated Without Surgery?
In most cases, TMD can be treated without surgical intervention. We always favor conservative options over invasive procedures if circumstances allow. However, some severe cases are best treated with surgery. If that is true in your case, we will walk you through the details of your recommended treatment plan so you can make a well-informed decision about how to move forward.
Is TMJ Treatment Expensive?
Because there are so many different TMJ treatments available, costs can vary greatly. Something like an occlusal splint or equilibration tends to have a lower cost than surgery. Surgery can also range in price, depending on how complex it is.
During your consultation, we will have an upfront discussion about the price of your recommended treatment plan. We will also be happy to walk you through your payment options, including financing and potential insurance coverage.
Keep in mind that even though some forms of TMJ treatment can seem expensive, they present an excellent value. After all, your health and quality of life are precious assets that deserve to be protected!
Wisdom Teeth Extractions Oral & Maxillofacial Pathology Oral Cancer Orthognathic Surgery Dental Implants Pre-Prosthetic Surgery Facial Trauma Treatment Apicoectomy Surgery Cleft Lip & Palate Surgery Corrective Orthodontic Surgery Sleep Apnea Treatment Anesthesia & Sedation Dentistry Cosmetic Facial Treatments Dental Emergencies View Our Services

