New Oral Surgery Patient Information Houston
What You Need to Know Before Your Visit
If you have an appointment at Piney Point Oral & Maxillofacial Surgery of Houston in the near future, know that our entire team is looking forward to helping you enhance your smile! You deserve to have your treatment go as smoothly as possible, so please review the information below before the date of your appointment. If there’s something you don’t understand or an issue you’d like to clear up ahead of time, get in touch with us right away, and our team will help you sort everything out.
Appointments

Because we realize that your time is valuable, we make every effort to see patients at appointed times. However, if an emergency situation arises that causes a delay or necessitates rescheduling your appointment, we will keep you well informed. If you find it necessary to change your appointments, we would appreciate as much advance notice as possible.
In general, most of our patients, even if referred to our office for a specific surgical service, will be seen for a comprehensive consultation visit before the date of surgery. The purpose of this visit is to allow you to meet your oral surgeon and discuss your diagnosis and oral treatment in a pleasant, stress-free environment. It is our experience that trying to have both the consultation as well as the surgery on the same day makes it difficult for some patients to make careful and considered decisions about their care.
There are, of course, exceptions to this, and some patients who are hurting or require urgent oral care will naturally be seen and treated on the same day. This is a decision best left up to the patient and oral surgeon. If you have any concerns or comments, feel free to discuss them at the time your appointment is made, or you may email us.
It would greatly assist us if, at the time of your initial consultation, you provide us with any or all of the following:
- Your referral paperwork and any X-rays from your dentist
- A list of your current medications, including dosages
- Insurance information to assist us in filing your claim
- Medical records
It will also assist us if you share whether you have a medical condition which may affect your care at the time of scheduling your consultation (these conditions include artificial heart valves or a history of rheumatic fever, heart murmurs requiring premedication, diabetes, hypertension, or heart disease).
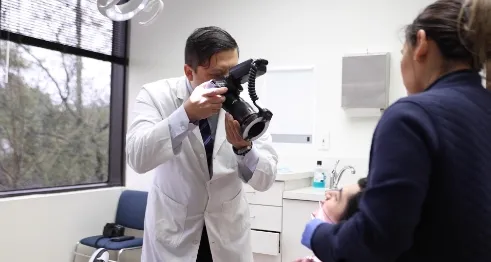
If your referring dentist has taken X-rays, you might request that these images be forwarded to our Houston oral surgery office in order to expedite your care. Additional images may be taken at our surgical office.
Patient Registration Forms

The below forms will need to be read and completed before you can have your first consultation with one of our oral surgeons. Instead of trying to hastily get everything done on the day of your appointment, you can print the necessary forms along with important information right here and review it on your own time. Then, when you walk into our oral surgery office for the first time, you can just hand us the completed paperwork.
View our Notice of Privacy Practices
Acknowledgement of Receipt of Notice of Privacy Practices
Your Consultation

Our oral surgeons will examine and evaluate your situation and discuss your oral surgery options with you during your consultation. This is a great time to become familiar with your surgeon and the staff and to voice your needs, questions, and concerns.
Your consultation will begin with a thorough review of your medical history and any existing X-rays. We ask that all patients please bring a list of medications they are taking, as well as the dosages. Following an overview of your health, our team will also discuss any associated fees for surgical services that you will be receiving, and our front desk staff will help conduct a benefits check with your dental or medical insurance plans.
If you are under 18 years old, you must be accompanied by a parent or legal guardian. We also ask that if you cannot keep your scheduled appointment, please let us know as soon as possible. We make every effort to see our patients at the appointed time, but we also understand that emergencies arise that can impact when we’re able to see you. In these cases, we will notify you of any delays.
Oral Surgical Fees & Payment

Our goal is to provide our patients with the highest quality of oral and maxillofacial surgical care. We strive to do this in a professional and businesslike environment, at a cost that is both fair and reasonable. Sending frequent statements and following up on delinquent accounts can be costly. Therefore, to avoid rising costs, we ask that all fees be paid at the time of service.
If special financial arrangements are necessary, please inform our front desk staff as soon as possible. For your convenience, we also accept Visa, MasterCard, Discover, and American Express credit cards. Additionally, we may be able to offer a third-party financing option for major elective surgeries that can ease the financial burden for these procedures.
We realize that medical and dental care is expensive. Our fees, by design, are within the usual and customary range for our specialty in this geographical area. Our front desk staff will outline any associated costs of your treatment with you beforehand to make sure that you have a clear idea of what you will be expected to pay out-of-pocket.
Medical & Dental Insurance Information

Many oral and maxillofacial procedures are covered by dental and/or medical insurance. It is very likely that you are insured under an individual or group policy that partially covers the type of advanced dental and oral surgery services provided in our office. However, it is extremely rare that a policy covers 100% of all charges incurred.
There may be deductibles, and frequently, insurance companies make payment on what they consider "usual and customary" fees for various oral and maxillofacial services. These payments may actually be lower than the fee charged. We do participate in many managed oral care (PPOs, HMOs, POS) programs. If you are a member of such a plan, please discuss this with our patient coordinator.
We will assist you in every way we can to see that you receive the maximum benefit allowable under your policy and expedite claims in a timely fashion. A standard "attending physician's" or "attending dentist's" statement will be provided and a form for predetermining benefits prior to the oral surgery will be supplied upon request. However, please remember that the patient is fully responsible for all fees charged by this oral surgery office regardless of medical or dental insurance coverage.