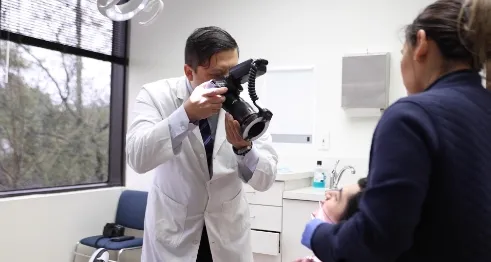
Tissue & Bone Engineering Houston
Improving Chances for Successful Dental Implant Placement
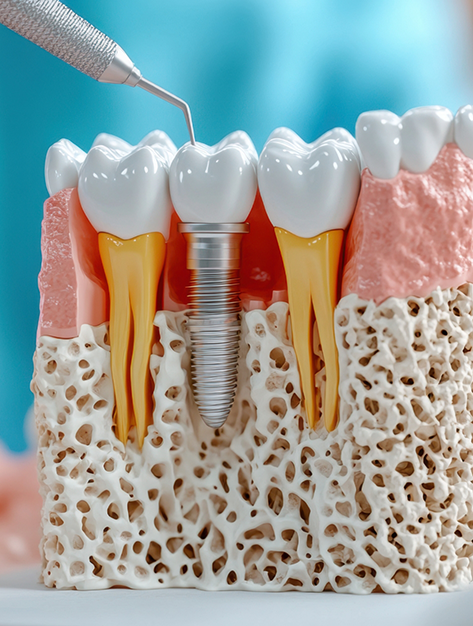
With the new advent of tissue and bone engineering technology coming into practical application, Piney Point Oral & Maxillofacial Surgery of Houston utilizes this technology with great success in multiple surgical applications. With this technology, the surgeons have been able to grow bone and tissue in severe defects to augment areas that would often require multiple surgeries to accomplish. With advances in tissue engineering technology, we can now add the benefits of molecular and biological factors to enhance the healing process, bone and soft tissue regeneration, and ultimately the outcome.
Surgical Tissue Engineering Techniques
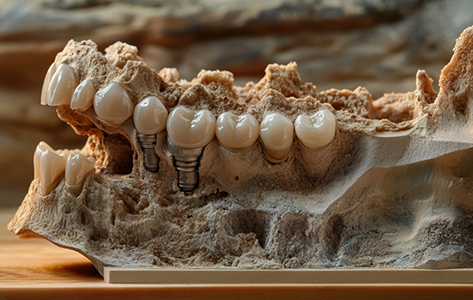
Here are the key tissue engineering techniques used in maxillofacial and dental implant surgery:
Platelet Rich Plasma (PRP)

PRP is derived from a patient’s own blood and is a concentrated platelet component containing various growth factors. It is added to bone graft material to enhance bone and soft tissue healing. These proteins have biological activity, among which are the growth factors to stimulate and speed up tissue regeneration. The process takes about 15 minutes, is safe, and does not lead to any side-effects.
rhPDGF
rhPDGF-BB stands for “recombinant human platelet-derived growth factor-BB.” It’s a completely synthetic grafting system designed to stimulate bone regeneration and wound healing when implanted into the body, like during dental implant placement and bone grafting. In fact, studies have shown that this method of surgical tissue engineering shows improved outcomes and offers unique advantages as compared to other more invasive surgical techniques.
rhBMP2
rhBMP2 stands for “recombinant (engineered) human bone morphogenetic protein-2.” It’s a genetically engineered version of a protein everyone’s body produces naturally in small amounts that can be used to help regulate bone growth and healing. rhBMP2 attracts the body’s own bone-building cells to the site and over time, new bone is formed. Bone grows where the rhBMP2 Bone Graft is placed, for predictable bone growth results.
Enamel Matrix Protein

This technology found its beginnings more than a decade ago when a breakthrough in the basic biology of tooth development revealed a native complex of enamel matrix proteins and the key role they play in the development of tooth-supporting tissues. As shown below, these “matrix proteins” mediate the formation of cellular cementum on the root of the developing tooth, providing a foundation for all of the necessary tissues associated with a true functional attachment.
Enamel matrix protein is comprised of a number of proteins that self-assemble to create a matrix. The dominant protein in this matrix is amelogenin, which has been remarkably well-conserved. This enamel matrix protein aids in the formation of new periodontal attachment in soft tissue to reduce the pocket depth of gums and help lead to more root coverage.
Benefits of Tissue & Bone Engineering Technology

For maxillofacial surgery, loss of bone or tissue in the face can occur due to multiple issues, including trauma, infection, pathology, etc. The use of the latest technology in tissue and bone engineering allows the oral surgery team to help increase healing, reduce post-operative complications, and improve integration of donor sites.
Bone and gum tissue loss, whether due to trauma or gum disease, has long been a limiting factor for patients seeking dental implants to replace their teeth. In such patients, bone grafting techniques allow us to restore missing or defective jawbone and create a stronger foundation for long-lasting dental implant-supported teeth. Common bone grafting procedures that we perform include extraction site bone grafting, onlay bone grafting, and sinus lift bone grafting.
The key challenges in today’s surgical success are primarily the speed, aesthetics, and the stability of the treatments in the long term. Tissue engineering and regeneration technology is an exciting and evolving science that helps us face such challenges with promising results.