Wisdom Tooth Extractions Houston
Comfortable, Gentle Wisdom Tooth Removal
Almost everyone will be faced with this question at some point, but the decision about whether or not to have wisdom teeth removed should be left up to you and your dentist. Your general dentist or an oral surgeon can help you evaluate the specific conditions of your wisdom teeth. Although many people benefit from the removal of their wisdom teeth, others may not derive significant benefits, and tooth removal may not be recommended.
Keep reading to learn everything you would want to know about wisdom tooth extractions, including their cost, when they’re necessary, and what you can expect from the procedure. If you have questions or want to schedule a consultation, contact the trusted oral surgeons at Piney Point Oral & Maxillofacial Surgery of Houston to learn more about wisdom tooth extractions in Houston.
Why Choose Piney Point Oral & Maxillofacial Surgery of Houston for Wisdom Tooth Extractions?
- Safe Dental Sedation for Comfortable Treatment
- Team of Highly Skilled Oral Surgeons
- We Accept Dental & Medical Insurance
What Are Wisdom Teeth?
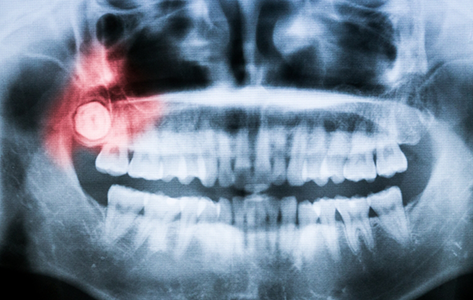
The wisdom teeth are actually a third set of molars at the very back of the mouth. These teeth may or may not erupt in late adolescence, usually between the ages of 16 and 24. If they do come through, there is rarely enough room for them to erupt (break through the gums) without issue. While ancient ancestors needed this third set of molars as their coarse diet and lack of oral hygiene often led to tooth loss early in life. Today, improved diet and the availability of preventive dental care means most people don’t need an additional set of molars, and there often isn’t room in the smile for these teeth to develop naturally. This lack of space can cause resulting oral health problems that range from minor to severe.
When Do Wisdom Teeth Need to Be Extracted?
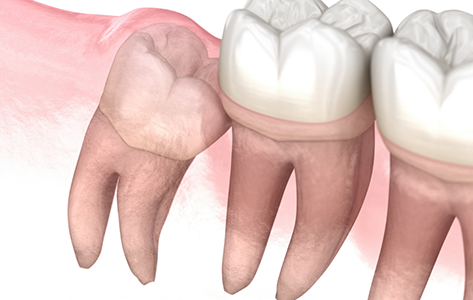
In order to determine whether you should have your wisdom teeth removed, you’ll need to visit our Houston oral surgeons for a tooth extraction consultation and exam. During this visit, we’ll capture digital X-rays and carefully examine your bite. We will be looking for concerns like impaction (teeth that can’t erupt), shifting in smile alignment, and assessing infection risk. We’ll also want you to tell us about any symptoms you’re experiencing associated with the development of your wisdom teeth.
Once we’ve gathered all the necessary information, we’ll sit down with you one-on-one to discuss your treatment options and determine whether or not wisdom tooth removal is necessary. We may recommend extraction based on the following reasons:
Read More About When Wisdom Teeth Need to Be Extracted
Overcrowding
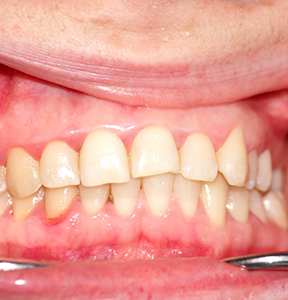
Around the time that wisdom teeth are coming in, many young people have just finished up orthodontic treatment to properly align their smiles. Some studies indicate that the development of third molars can lead to overcrowding and undo the effects of orthodontic treatments. If lack of space in the smile has the potential to cause misalignment or lead to impaction, wisdom teeth removal will likely be recommended.
Path of Eruption
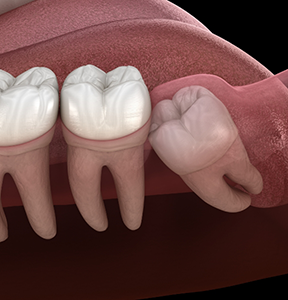
Another concern connected to smile alignment is the wisdom tooth’s path of eruption. Most permanent teeth follow the path of eruption from the primary teeth, but wisdom teeth don’t have a path to follow. For some people, this means the teeth erupt in improper alignment with the rest of the smile, or the teeth may be crooked within the socket when they erupt. In some cases, the wisdom teeth will even develop facing toward the surrounding teeth, which can lead to impaction or cause the smile to shift.
Infection

About 25-30% of wisdom teeth are removed due to pericoronitis. This is a localized infection of the gingival tissues (gums) associated with a partially erupted wisdom tooth, and it usually causes significant discomfort. In certain situations, this localized infection may spread and result in a more serious and even life-threatening infection called cellulitis.
Treatment of pericoronitis usually involves the removal of both the upper and lower wisdom teeth. The upper wisdom tooth is removed because it impinges on the swollen gum tissue around the lower wisdom tooth. Due to the difficult if not impossible task of properly brushing and flossing around a partially erupted wisdom tooth, they are at greater risk of infection, and these teeth will more frequently develop dental decay (cavities) or periodontal (gum) disease.
Impaction
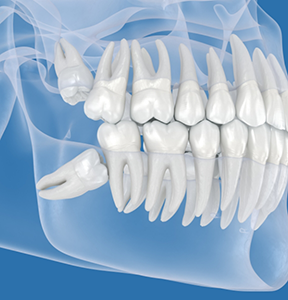
The term “impacted” describes a tooth that does not fully erupt from the gums. Wisdom teeth may be fully impacted, which means that the crown never breaks through the gum surface, or they may be partially impacted, which means only part of the tooth erupts. Impaction typically occurs because the mouth is too small to accommodate the wisdom teeth.
Impacted wisdom teeth have the potential to cause a number of serious dental complications, including increased risk of tooth decay and infection, potential to damage other teeth and oral structures, and possibility of shifting the smile out of alignment. Additionally, a cyst may develop around the impacted tooth, leading to nerve, jawbone, or tooth damage.
Though wisdom tooth impaction does not always necessitate extraction, it is a condition that should be thoroughly evaluated to determine the overall effect on the rest of the mouth before it becomes a severe problem.
Sinus & Airway Issues

The sinuses are the pockets of air located in the skull and facial region. They make it easy to breathe, trap pollutants in the air, improve speech, and lighten the weight of the skull. A sinus infection occurs when these spaces of air become inflamed. This type of infection is painful and may make it difficult to breathe.
The wisdom teeth in the upper back jaw are close in proximity to the maxillary sinuses just behind the nose. When they start to grow in, the roots and teeth may place pressure on this area, which can lead to sinus headaches or infections. Taking the wisdom teeth out completely will remove the pressure from the sinuses, alleviating tension headaches, jaw pain, and other symptoms.
Pathological Conditions (Cysts & Tumors)
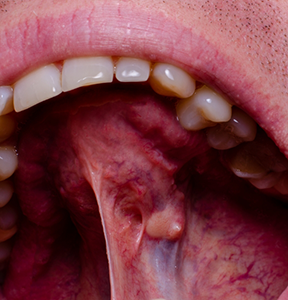
Approximately 1-2% of wisdom teeth are removed because of pathological conditions such as cysts or tumors. Although 1-2% sounds like a very low probability, 10,000 - 20,000 people out of one million will have some type of pathological condition associated with their wisdom teeth. Most of these conditions can be detected during routine dental exams through panoramic dental X-rays, and this is one reason that patients are recommended to have a panoramic X-ray taken every three to five years.
Wisdom Teeth & Sinus Issues
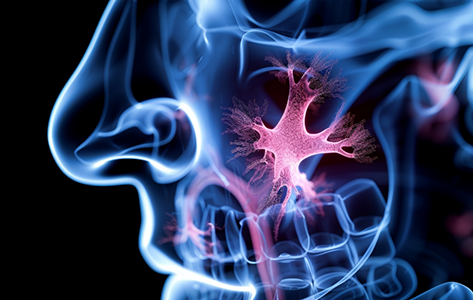
The wisdom teeth are a set of third molars that typically try to erupt during late adolescence or early adulthood. Most people have them -- and in many cases, these “extra” teeth can cause a lot of issues for your oral and overall health. The sinuses are one example; wisdom teeth may place pressure on this area and ultimately cause pain or sinus infections, among other side effects. In these cases, your oral surgeon in Houston can help with wisdom tooth extraction. Learn more about how wisdom teeth can affect sinuses by clicking on the button below.
Read More About Wisdom Teeth & Sinus Issues
The Link Between the Wisdom Teeth and Sinuses
The sinuses are empty pockets of air that are located in the skull and facial region. They make it easy to breathe -- and there are sets in the forehead, inside the cheekbones, and behind the nose.
A sinus infection occurs when these spaces of air become inflamed. This type of infection is painful and may make it difficult to breathe.
Oral health is closely related to overall health, and one clear example is between the wisdom teeth and sinuses. The wisdom teeth in the upper back jaw are close in proximity to the sinuses located behind the nose. When they start to grow in, the roots and teeth may place pressure on this area -- which can, in some cases, lead to sinus headaches or even sinus infections.
How Wisdom Tooth Extraction Helps

Wisdom tooth extraction is a common oral procedure that can take away the problem causing sinus infection or any of the other issues related to impaction (like discomfort in the jaw, shifting teeth, etc.).
General dentists will not recommend surgery unless they are sure it’s necessary -- so first, X-rays and a thorough examination will be completed to determine the placement of the wisdom teeth and confirm that they are the cause of any sinus troubles. Once this has been identified, a separate appointment for extraction will be made.
Taking the wisdom teeth out completely will remove the pressure from the sinuses, reducing pressure and alleviating tension headaches and jaw pain. That means at long last, relief may be in sight!
What to Expect from Wisdom Tooth Extraction

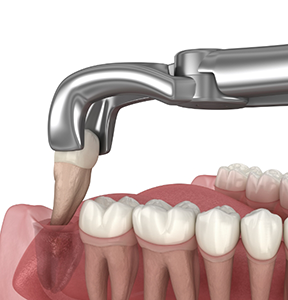
The extraction procedure itself will vary depending on your unique case. In some situations, teeth can be removed using traditional tooth extraction techniques. More commonly, wisdom teeth are sectioned, separated into smaller pieces, then removed one piece at a time. The advantages of this technique is that since bone removal is minimized, you will generally heal more rapidly and will have less discomfort following the surgery.
Read More About What to Expect
Preparing for Your Wisdom Tooth Extraction Procedure

If you and your oral surgeon decide that wisdom tooth extraction is the right option for your smile, you’ll receive a personalized treatment plan, including preoperative instructions. You can also review pre-op instructions page to learn more. The basics to keep in mind include:
- Clean your teeth immediately before your appointment.
- You should be accompanied by a responsible adult who can drive you to and from the appointment and monitor you during recovery. Legal minors must be accompanied by a parent or guardian.
- You should have nothing to eat or drink for at least six hours prior to surgery. If you have to take sedative medication from the oral surgeon, it should be taken with only a sip of water.
- Wear loose-fitting clothing and short sleeves. Do not wear tight collars, jewelry, or neckties.
- The most significant sedative effects wear off within an hour of treatment, but residual effects can last from 12 to 24 hours after the procedure.
Dental Sedation & Anesthesia Options
To ensure you maintain comfort throughout the most complex surgical tooth removal, your oral surgeons use a range of dental sedation and anesthesia options. Their recommendations will depend on your specific case, but at Piney Point Oral & Maxillofacial Surgery of Houston, the team is able to offer a full range of options from the mildest combination of local anesthesia and nitrous oxide (laughing gas) to IV sedation, also referred to as sleep dentistry.
Treatment Locations
Depending on the complexity of the procedure, the team at Piney Point Oral & Maxillofacial Surgery of Houston may be able to perform your wisdom tooth extraction in-office. Your trusted oral surgeons in Houston also provide more advanced surgical treatments at local hospitals to ensure your safety during the procedure. The complexity typically depends on the angle and location of the wisdom teeth and whether or not the teeth have erupted through the gums.
Tooth Extraction Procedure
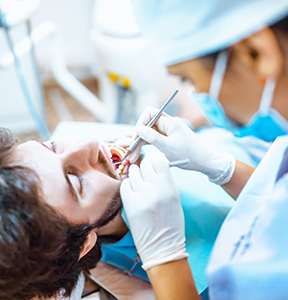
The length of your wisdom tooth extraction surgery will be dependent upon the complexity of your case. If wisdom teeth have fully erupted, the oral surgeons at Piney Point Oral & Maxillofacial Surgery of Houston may be able to pull them, which can be done relatively quickly.
For fully or partially impacted wisdom teeth, those that have become fully fused with the supportive structures, or teeth close to nerve structure that impedes ability to remove the tooth, surgical extraction will be necessary. These more advanced procedures can take several hours. Before the day of your appointment, the team will let you know what the estimated surgical time is for your specific tooth extraction procedure.
Coronectomy
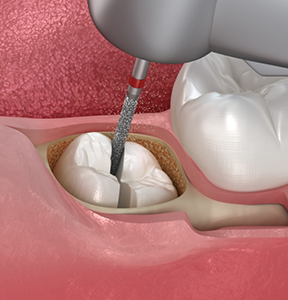
Normally, a wisdom tooth extraction involves taking the entire tooth out of the mouth, but this is not always necessary. If a wisdom tooth has healthy roots that aren’t causing any problems, or if the roots are positioned very close to a sensitive nerve, your oral surgeons in Houston may perform what is called a coronectomy. The crown, or upper portion of the tooth, is separated from the roots and removed, while the roots are left in place. This makes the procedure much less invasive, leading to a faster and more comfortable recovery.
Aftercare & Healing Following Wisdom Tooth Extraction

Following wisdom tooth extraction, you should expect to experience certain normal postoperative symptoms. These symptoms include mild to moderate bleeding that should decrease over the first few hours, but mild "oozing" from the extraction sites may continue for up to two days. Also, you’ll likely experience some swelling, especially in the lower jaw, which may increase for two to three days postoperatively. Swelling should slowly start to resolve over the next week to ten days.
It is normal to experience limitation to your range of jaw movement and discomfort with chewing. After removal of wisdom teeth, you will be given a set of postoperative instructions specific to your situation. You can also find general aftercare instructions on this website. In most cases, oral surgeons recommend following the basic post-op care routine:
Read More About Aftercare & Healing
First Day After Tooth Extraction

- Medications – Antibiotics and anti-inflammatory medications should be continued as directed and pain medication taken as needed.
- Ice Packs – Ice packs should be used at 10-minute intervals throughout the first day, and it is not unusual to have increased swelling on the first day after surgery.
- Diet – Full liquid diet should be continued throughout the day.
- Oral hygiene – Begin brushing teeth the first day after surgery, carefully avoiding the surgical sites until after the follow-up visit.
Second Day After Tooth Extraction

- Medications – Antibiotics and anti-inflammatory medications should be continued as directed and pain medication taken as needed.
- Ice Packs – Ice packs should not be used the second day after surgery.
- Diet – A soft food diet may be started. This can include foods like scrambled eggs, mashed potatoes, and other items of similar consistency.
Third Day After Tooth Extractions

- Medications – Antibiotics should be continued until the entire prescription has been taken. Anti-inflammatory medication may be discontinued unless needed for relief of discomfort. Pain medication should be taken only if full relief of discomfort is not achieved with the anti-inflammatory medication.
- Heat – If symptoms of swelling, bruising, or stiffness are present, apply a heating pad or moist heat to the affected area three to four times daily for approximately 20 to 30 minutes each time. Heat should be continued until the symptoms subside, which may take several days.
- Diet – Continue eating softer foods and reintroduce more difficult-to-chew foods as you feel comfortable, taking care to avoid the surgical site when chewing.
Dental Emergencies During Recovery
Proper care following oral surgery will hasten recovery and prevent complication. Although tenderness is not unusual for several days, you should feel progressively better every day starting three to four days after your surgery. Regular postoperative visits are scheduled for five to 10 days following surgery, but if severe throbbing pain or pain unrelieved by medication persists, please notify the oral surgery office immediately. Your oral surgeons in Houston may ask you to come in sooner.
Possible Complications After Wisdom Tooth Extraction

By following the post-operative care instructions, you can typically make a full recovery without concern, but there are some complications associated with this surgical treatment. The team has outlined the most common complications that occur after wisdom tooth extraction below, but feel free to contact the office if you’re concerned. If any unusual symptoms occur, you may reach your oral surgeon 24 hours a day by calling (832) 293-4912.
Read More About Possible Complications
Dry Socket
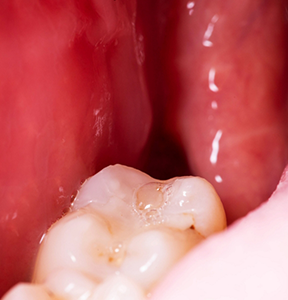
Following a tooth extraction, a blood clot forms over the top of the extraction site to promote healing and protect the sensitive nerve structure below. If this blood clot fails to form, breaks down too quickly, or becomes dislodged, patients may experience dry socket. This common postoperative complication, also called alveolar osteitis, affects between 3% and 25% of people.
The treatment of dry socket consists of washing out the socket with a saline solution that removes food particles and bacteria buildup and placing a medicated packing into the socket. This usually provides significant relief of symptoms within an hour. The packing is removed after five to seven days.
Your oral surgeon might also provide a medicated mouth rinse that you should use for several days to keep bacteria from the area and promote faster healing. The occurrence of dry socket will not affect the final quality of healing, but it can extend the length of healing time and cause significant discomfort.
Infection

Although postoperative infections after the removal of wisdom teeth are rare, any infection left without treatment can become severe. As stated above, one of the reasons you may have your wisdom teeth removed is because of infection. Therefore, you may already have an infection associated with your wisdom teeth at the time of surgery. Even after the removal of wisdom teeth, you may require further treatment to resolve the infection, which could include taking antibiotic pills and/or using an antimicrobial oral rinse.
Rarely, you may develop a chronic, low-grade infection of the bone at the extraction site, even weeks after the tooth was removed. This chronic infection of the bone (osteomyelitis) may require further antibiotic therapy and/or surgical debridement.
Numbness

Due to the proximity of the wisdom teeth to the various nerves in the jaw, the removal of these teeth has been associated with a 1-3% incidence of temporary numbness to the lips, gums, teeth, or tongue. The majority of temporary numbness occurs in the lower lip and may last four to six weeks. A very small percentage of people experience a permanent sensory deficit in these areas. In the rare cases of permanent changes in sensation, it should be noted that you do not look different, drool, or talk differently.
Of the areas at risk, the tongue can be the most bothersome to you, potentially affecting taste. If you experience numbness of the tongue without improvement after four to six weeks, consideration may be given to exploration and repair of the nerve.
Less Common Complications

Other complications associated with the removal of wisdom teeth include damage to adjacent teeth, displacement of upper wisdom teeth into the maxillary sinuses, thermal sensitivity to adjacent teeth, pain or dysfunction of the jaw joint (TMJ), and limited ability to open and close the mouth. Sinus complications including infection occur rarely and may require additional treatment or surgery.
Understanding the Cost of Wisdom Tooth Extraction

The cost of wisdom tooth removal will vary based on several key factors. These include the number of wisdom teeth being extracted, as you may not have all four wisdom teeth. It will also depend on whether your tooth or teeth are impacted (stuck under the gums or partially emerged), as well as the formation of the oral structures and tissues around it. The type of sedation used during your procedure in addition to the local anesthetic will also influence the cost of removing your wisdom teeth.
After examining your mouth and outlining your treatment plan, the team will provide you with a detailed cost estimate and factor in any insurance benefits that may apply. The team will also walk you through financing and additional payment options if needed.
Read More About The Cost of Wisdom Tooth Extraction
What Is the Typical Cost of Wisdom Tooth Extraction?

The cost of a wisdom tooth extraction will vary based on how many teeth are being removed, the complexity of the case, the cost of the initial exam, X-rays, and sedation. Typically, the range you can expect for these factors is as follows:
- Extraction per tooth: $292 to $1,000 (depending on the complexity of the case)
- Total for removing all 4 wisdom teeth:$616 to $5,950
- Exam and X-rays: $0 (included) to $502
- Sedation: $97 to $600 (depending on the type, such as nitrous oxide or IV sedation)
Does Dental Insurance Cover Wisdom Tooth Extraction?

Most dental insurance policies offer some level of coverage for wisdom tooth removal. Since it’s often classified as a “major procedure,” you can typically expect your dental insurance to cover 50-80% of the cost. However, it’s important to remember that every insurance plan offers different benefits, so you should investigate the details of your policy or contact your insurance provider to learn more about your coverage. The cost of your wisdom tooth extraction will also likely be influenced by your yearly maximum and deductible.
We’re proud to accept a number of popular dental insurance policies. The team at Piney Point Oral & Maxillofacial Surgery of Houston has years of experience navigating the details of various plans and would be happy to help you review your benefits to learn more about your coverage for wisdom tooth extraction.
Affordable Payment Options & Financing

Dental insurance benefits can offer a tremendous amount of assistance in terms of lowering your out-of-pocket cost for wisdom tooth removal. Additionally, many patients qualify for no-interest financing. This would allow you to break up the cost of your treatment into smaller, more manageable payments that fit easily into your monthly budget.
Comparing Wisdom Tooth Extraction Costs Between Houston Dentists

When shopping around for who to trust your smile to, remember that cheaper is not always better. Here are a few important things to keep in mind when comparing prices:
- Beware of suspiciously low-priced tooth extractions. These are likely only advertising the price of one part of your treatment, leaving you with unexpected costs along the way.
- Lower prices for wisdom tooth removal may only be for simple extractions, whereas more complex cases or impacted wisdom teeth will naturally cost more.
- Seeing a highly trained oral surgeon for wisdom tooth removal may cost more than a general dentist, but you should never entrust your oral health to a professional who doesn’t have the right experience or training for your unique situation, especially if you have a complicated case.
General Dentist vs. Oral Surgeon: Who Should You See to Have Your Wisdom Teeth Removed?

In some cases, a general or family dentist can extract wisdom teeth. However, many dentists choose to refer their patients to a trusted oral surgeon instead, especially in more complex, severe, or impacted cases.
Oral surgeons have years of advanced training in tooth extractions and other serious procedures, and since wisdom teeth are the most commonly removed teeth, oral surgeons are well-versed in how to perform wisdom tooth extractions. They are also more likely to have training and certification in sedation dentistry options, such as IV sedation, than a general dentist, which can ensure that your treatment goes smoothly and comfortably.
Remember, your dentist may recommend wisdom tooth removal even if you can’t see or feel them yet. Even if your wisdom teeth aren’t bothering you right now, having them extracted will likely save you the time and money of dealing with complications in the future.
Wisdom Tooth Extraction FAQs
At What Age Should Wisdom Teeth Be Removed?
Many people have their wisdom teeth removed between the ages of 17 and 25, before the bone develops to the point where extraction may be more difficult. However, there are no set-in-stone rules for when wisdom teeth should be removed. Patients older than 25 often have successful extraction procedures.
What Factors Should I Consider When I’m Deciding Whether or Not to Get My Wisdom Teeth Extracted?
Keep in mind that wisdom teeth extractions aren’t necessary for everyone. When deciding whether you should undergo this procedure, you should listen to your general dentist or oral surgeon’s advice. If they believe your third molars are currently posing a threat to your oral health or they may do so in the near future, extraction is likely the wisest choice.
Some patients have their wisdom teeth removed as a purely preventive measure. If you are thinking about doing this, be sure to thoroughly discuss the risks and rewards of the procedure with an experienced oral surgeon before you make your final decision.
What Symptoms Indicate That I Might Need Wisdom Teeth Extractions?
Some signs that indicate you should visit your dentist to discuss wisdom teeth extractions include:
- Soreness in the jaw (especially toward the back of the mouth)
- Gum problems around the wisdom teeth
- Pain in the wisdom teeth or the teeth next to them
- Difficulty keeping the wisdom teeth clean
Is Wisdom Tooth Extraction Painful?
Thanks to local anesthesia, sedation dentistry, and general anesthesia options, you can expect to feel nothing during the extraction surgery. However, you’re likely to experience some swelling and soreness afterward. Your oral surgeon in Houston will give you detailed post-operative instructions that will help to minimize your discomfort and make your recovery as smooth and efficient as possible. You should be back to feeling like your old self within one to two weeks.
How Much Does Wisdom Teeth Removal Cost?
The cost of wisdom tooth extraction in Houston will depend on many factors, including:
- The number of wisdom teeth that are being extracted.
- The complexity of the procedure (whether or not the teeth are impacted as well as the formation of the oral structures around them).
- The type of sedation used (general anesthesia or IV sedation costs more than local pain-numbing methods).
Oral & Maxillofacial Pathology Oral Cancer Screenings Orthognathic Surgery Dental Implants Pre-Prosthetic Surgery Facial Trauma Treatment Apicoectomy Surgery Cleft Lip & Palate Surgery TMJ Treatment Corrective Orthodontic Surgery Sleep Apnea Treatment Cosmetic Facial Treatments Anesthesia & Sedation Dentistry Emergency Dentistry View Our Services